
The best way to get the most out of our NHS is to compare it with health systems across Europe – and how they pay their workers.
Everyone knows the truism. The NHS is a national religion. Every other institution is known by its name, if it’s known at all. But the health service is “our” NHS. The people who work for it aren’t staff, they’re called “heroes”. During the pandemic, ministers made sure they were seen by the TV cameras outside their house clapping, like hostages to public opinion being wheeled out to act out their loyalties.
But public affirmations of faith are easy. Private conviction is another matter altogether. Last week, we saw that tension play out. The government delivered a double-blow to the NHS. One was expressed by absence, the other sneaked out in the dead of night when they thought no-one was watching.
The first came when Rishi Sunak unveiled his Budget last week. Despite years of inadequate funding and a Covid emergency, there was barely a mention of the health service. No long-term plan. No vision. A black hole in a red box.
The second attack came the next day, with a one per cent pay rise for NHS workers. In reality, with inflation expected to be 1.5% next year, it amounted to a real terms pay cut. The decision – and the manner in which it was surreptitiously announced – communicated a sense of how ministers talked about the NHS when they were behind closed doors, which was a million miles away from the pieties they utter on camera.
The reaction since then has been predictable: high-pitched, full volume moral outrage. It’s the kind of reaction which is typical of religious controversy and it’s largely justified. But the sound and the fury threatens to prevent us from taking a more forensic, objective look at the health service. What are we doing wrong? What are we doing right? How do we compare with other countries? What can we learn from them?
It’s worth comparing NHS performance with health policy data from Europe. The most reliable data we have on international health spending and nurses’ pay comes from the Organisation for Economic Co-operation and Development (OECD). It shows that UK health care spending is about average for its 35 members and the EU’s 27 member states.
But that’s not a particularly revealing exercise. That analysis includes many low-income countries, like Latvia, which the UK wouldn’t normally compare itself to. A much better approach is to contrast it with high-income European countries like Germany, the Netherlands or Sweden.
When you do that, the true pattern reveals itself. The UK is consistently one of the lowest spenders on health care in this category. Switzerland allocates 12.1% of its GDP to health, Germany 11.7% and France 11.2%. Britain spends just 8.7%.
You can see that in capital investment. This is what dictates the resources available to staff to deliver care for patients. Between 2000 and 2017, while other countries delivered sustained rises, the value of capital per health care worker in the UK fell by 35%.
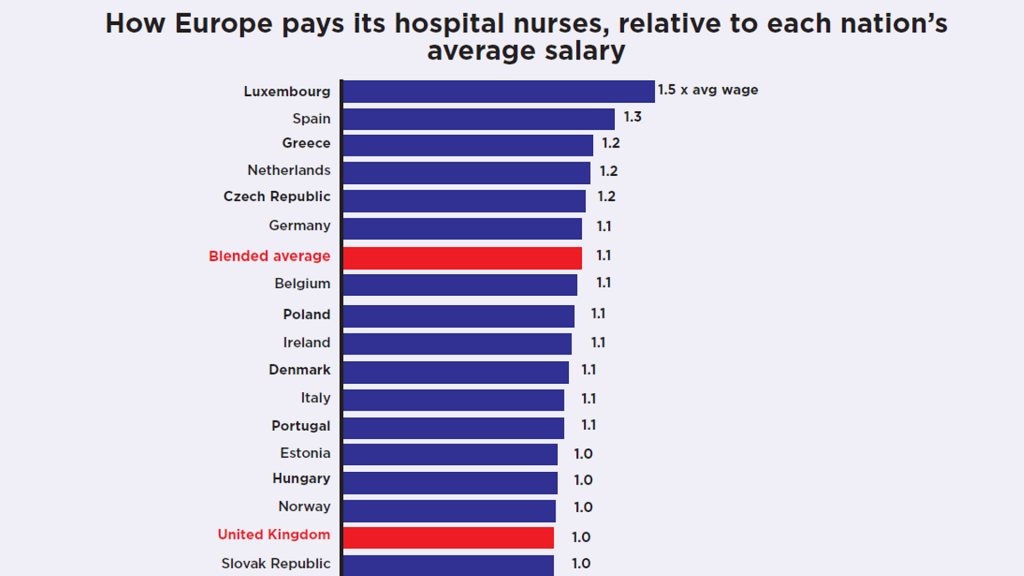
Compared to average wages, nurses in the UK are paid less than those in Spain, the Netherlands, Germany, Belgium, Ireland, Denmark, Italy, Portugal or Norway.
The number of practising nurses per 1,000 people in the population is 7.8 in the UK, compared to 11.4 in comparable countries. To make matters worse, the existing workforce is quite old, meaning large parts of it are about to enter retirement.
Brexit made this problem much more severe. In the years after the vote, many European nurses in the UK – particularly in London and the South East – grew uncomfortable. They read the newspapers, which treated them like a problem. They saw the referendum result, which suggested the public agreed. They looked at their salary, which was often less than in their home country. And they asked themselves: Why stay?
Many couldn’t find an answer to that question. More than 3,000 EU nurses left the NHS in 2017 alone. This was combined with an 87% drop in new nurses coming from the EU to the UK between 2016 and 2018.
Lack of funding and reduced staffing translates into worse care. Britain has fewer hospital beds per population than comparable countries. It has a lower life expectancy. It has a greater average rate of preventable deaths. It has the lowest survival rates for breast cancer and colon cancer and the second lowest for rectal cancer and cervical cancer.
But even putting aside expenditure, a European comparison raises troubling questions about how the NHS works. They come down to its funding model and its highly centralised structure.
Having a taxpayer-funded health service is core to the NHS’ domestic appeal. No politician who wants to maintain their career is foolish enough to question it. But it’s notable how few European countries have emulated this approach. Germany, the Netherlands and France, for instance, have an insurance-based model.
Insurance-based models put an emphasis on preventing disease rather than treating it, for the simple reason that it’s cheaper for the companies involved. They therefore tend to encourage regular visits to specialists like paediatricians and gynecologists.
Britain has a terrible record in this area. Instead of encouraging preventative appointments, we focus on treatment. And this is key to our poor performance on cancer. It means that people usually go to see their GP once they see symptoms. But by then it is often too late.
The same applies to centralisation. Most European healthcare is delivered by local regions rather than from the capital, as it is in England.
You could see the effects of that play out during the pandemic. In Germany, health decision-makers were making choices about regions they lived in and understood. In England, those decisions were made in London, about places those people had never visited. A lot gets lost in that distance.
But this isn’t a simple story. There are advantages and disadvantages to each approach. Covid also revealed some of the strengths of a highly centralised – and therefore highly integrated – health system.
Look for instance at the Lombardy region of Italy. It was devastated by coronavirus, experiencing a much higher per capita infection and death rate than any other part of the country. Many experts believe that was because of the way its health system is organised.
Since the late 1990s, Italian healthcare has been decentralised, giving regions more autonomy. Lombardy’s governors – like Silvio Berlusconi’s Forza Italia and Matteo Salvini’s Lega – used that power to introduce extensive private provision to compete with public providers. That created a situation where communications about the virus often stalled, making an organised response harder to manage.
There are other advantages to the British system. That much is obvious by how few people in the UK have private health insurance. Many European countries, like Spain or Greece, have huge numbers of people going private. In the UK, it’s around 6%. That is a mark of confidence in the NHS. The middle classes in Britain, unlike many of its continental neighbours, choose to stick with state-provided healthcare.
The European insurance model also has significant flaws. Given how little Britain spends, health outcomes should really be much worse than they are. The fact that they’re not speaks to two things: the commitment of NHS staff to deliver the best care they can and the level of cost-effectiveness in a tax-funded, free-at-the-point-of-use health service.
Insurance models tend to spend a lot of money in administrative costs. This is much less of a problem in the NHS.
But that doesn’t mean we can’t learn from Europe. When it comes to preventive measures, we can use cultural initiatives to accomplish what other countries do with financial incentives.
That involves a major change. We have to get rid of the idea that the less you use the health system, the better. Instead, we should adopt a European assumption that regular check-up appointments are a normal part of life. That change should come from ministers. But failing that, it can come from the bottom-up through a demonstration of demand from voters.
The most important lesson Britain can learn from comparable European countries ultimately comes down to money. We need to invest in infrastructure and technology, with a long-term plan to manage health and social care with an aging population.
We also need to invest in people. This comes down to both staffing and pay. A nurse’s productivity is not just about health outcomes. It’s about having time to make people feel better. It’s about having the capacity to provide comfort. That cannot be achieved if we continue to allow the staff-to-patient ratio to decline.
Most nurses aren’t ultimately motivated by the money. But they do need to feel that they are valued. You can’t do that if their pay falls compared to that of other sectors. You can’t do it if you have a prime minister who stands outside clapping for the cameras only to then retreat indoors and sign off on a de-facto pay cut.
Our current approach sends a clear message: You’re not valued. You’re not worth it. And by doing that we encourage nurses to leave the profession and young people not to join in the first place. That then makes the staff-to-patient ratio even worse.
You have to show you value people. Not just by saying it, but by delivering on it. It’s a very simple lesson. But it’s one the government is apparently incapable of learning.
What do you think? Have your say on this and more by emailing letters@theneweuropean.co.uk










