So according to the generals in government, the war on Covid is all but over. But is it? To the foot soldiers here on the frontline, it still feels like a battle, in many cases between life and death.
Forgive the war analogies, but alongside the dreadful events in Ukraine, inevitably the pandemic is slipping out of the public debate, and it is important we do not lose sight of the challenges ahead, not merely the gains made. Leaders for whom for two years Covid has been the Number 1 priority now find their attention taken elsewhere, as it should be. But Covid does not care about the news agenda, or politics, and my experience as a doctor in one of London’s busiest Intensive Care Units leads me to be hopeful we have turned a corner, but humble and cautious in the face of an enemy that has outwitted us before, and might do so again.
When I first saw the images from intensive care units in Lombardy at the end of February 2020 I realised that I’d be facing one of the biggest challenges of my career over the months which followed. Looking back I was fantastically naive about what lay ahead.
Before it hit, my anxiety was all about the potential scale of the problem (mingled with fears about the risk to my own health). Some models suggested that we’d need an extra 4,000 ICU beds in London alone so a group came up with concept of the Nightingale Hospital, a 4,000 bedded makeshift ICU in the Excel Centre. Three weeks later it was built. Impressive. But it turned out to be of little use. It was designed on the prediction that we’d have hundreds of patients in respiratory failure who would need basic ventilation for a week or two, and then be fine.
But by the time the Nightingale opened to great fanfare, it was clear that that couldn’t be further from the truth. Covid patients turned out to be the sickest, most unstable and unpredictable group we’d ever looked after. They didn’t just need ICU, they needed state of the art ICU – and even then more than a third of them died. The Nightingale model, with fewer trained staff and basic ventilators was not going to work. Covid had just served up its first of many big surprises and a change of strategy was needed.
Fortunately, although we locked down late it was in time to avoid the requirement for all 4,000 extra ICU beds and we managed to keep the vast majority of critically sick patients within established hospitals. Our ICU like many others more than tripled in size and filled up with patients from around London, many of whom needed multiple organ support and daily turning on to their front just to stay alive.
As the patients rolled in through the front door it felt like a battle zone, but a far more complex one and than we’d foreseen. This was about so much more than just the scale and our safety. We hadn’t even considered the plight of the relatives, we didn’t know how to redeploy all of the willing but untrained staff from other departments, we had no idea how we would distribute such complex patients around the different hospitals, we didn’t know if we would have enough equipment or oxygen and we hadn’t worked out how to divide up the hospital between covid, possible covid and non covid patients. Worst of all we didn’t know the best way to manage this awful disease. How and when should we ventilate Covid patients? Which drugs should we use? Should we thin their blood? Should we use the tight CPAP masks? When should we put in tracheostomies? No-one knew the definitive answers to any of these questions and so different hospitals tried radically different approaches. It was unnerving. What if our approach turned out to be wrong? We might have double the mortality of other units – and the patients weren’t all elderly and infirm. My first Covid death was a previously fit and well painter and decorator. He was 28 years old. I have seen much death in my work. This one really hit me.
Gradually over the weeks we learnt. We saw patterns emerge, we shared information with other units, we built teams, we collected data, we wrote guidelines and we ran trials that picked out the effective interventions. The world was working it out together, but as the first wave petered out there was still so much we didn’t know. Would it come back? Would we create a vaccine in time? Would it mutate? Would it be worse next time? Would we all catch it eventually? Would it be with us forever?
My brother had encouraged me to keep a diary throughout the pandemic and when I came up for breath from those awful few months, I sat down to write a book, ‘Life Support.’ It helped me try to make sense of what we had been through, and think more deeply about those questions as we wondered what the next phase might look like. I couldn’t imagine going through it all again, but equally I couldn’t believe that people would be able to launch safe and effective vaccines within a year. I should have given the scientists (and the virus) more credit.
Through the autumn of 2020 I contacted the patients and relatives that I had written about to ask for their permission. Normally once patients leave the unit I never see them again so this was educational, as well as moving and inspiring. The relatives of the deceased were still processing their grief, but they were universally generous and spoke at length about their loved ones. They also taught me what an impact small acts of kindness have at our darkest moments. Relatives could hardly visit during the pandemic so we had to update them by telephone. Many of them sat waiting all day for our call, terrified they’d miss it. Occasionally the team were overwhelmed and the call was never made, so we set up a dedicated family liaison team who ensured that everyone was contacted by a certain hour each day. The team then organised video calls so that the families could see their loved ones. I was sceptical at first. I thought it all sounded a bit morbid. Who’d want to look through an i-pad at their unconscious husband lying face down on a ventilator? I couldn’t have been more wrong. The families told me it was a lifeline, because it gave them at least some insight into what was going on. Now they could see the care and dedication of the staff and feel comforted that someone was looking after their relative, even if they couldn’t be there. They’d had visions of them dying alone. The last thing they’d seen was their relative being taken away in the back of an ambulance.
The patients I spoke to were extraordinary. I’d watched every one of them cling to life for weeks. I’d discussed them repeatedly with colleagues, pondering whether there was any chance left they’d recover. I’d felt helpless and often considered that it might be kinder to let nature take its course, but now I was talking to them on the telephone. They were home and they were delighted to be alive. They still had problems, but many were back at work (some in the NHS) and one had a pregnant wife who delivered a beautiful healthy baby girl 6 months later. At last all those dark days (and nights) seemed worth it – and then the second wave hit.
I found the second surge even harder. We were much better prepared and organised, but foolishly this time I thought we’d be able to make (almost) everybody better. I’d seen people recover from seemingly hopeless positions the first time round and I thought that if we just used everything we knew and kept going, however bad it looked, eventually they’d turn the corner and get better. But of course many didn’t. The patients hadn’t died the first time because we’d given up on them, they’d died because Covid is a vicious, relentless disease.
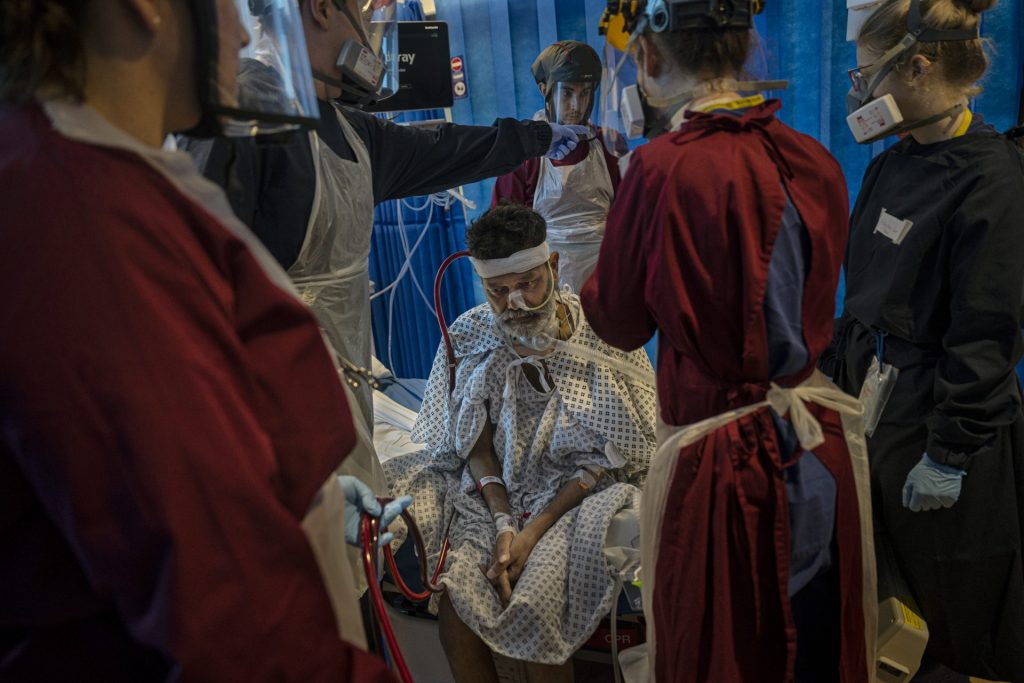
But that second surge died away in Spring 2021 and by now we had the vaccines. I dared to hope again that it might all come to an end. Gradually through the summer the country unlocked. Ironically my two children tested positive on so-called ‘Freedom Day’, July 19th 2021, but after a few days of screens-in-bed therapy they got better. Through the Autumn our steady stream of critically sick Covid patients were almost all unvaccinated and while that was frustrating it was also reassuring. It showed the vaccines were working.
Then Omicron struck and all bets were off. What havoc would this new, more infectious strain wreak? As Boris Johnson gambled on keeping things open we all prepared for the worst. We wrote emergency rotas, warned our families that we might not be around much over Christmas and prepared for another surge of ICU cases. Thankfully, it never came. He and we got lucky. This most unpredictable of pathogens had let us off relatively lightly – this time.
And then suddenly it was ‘all over.’ There were still 40,000 cases per day, but all the rules had gone. There was no necessity to wear masks anywhere, no free tests (unless you were vulnerable, but not if you looked after the vulnerable) and no need to isolate if you tested positive – just ‘use your common sense.’ The scientists were saying there would likely be more ‘variants of concern,’ and we knew that Omicron was still circulating at high levels and a risk to vulnerable people, but nevertheless everyone could do what they wanted. We had to learn to live with Covid and that meant going back to normal. The government told us that our response and our world beating vaccine programme had saved the day and allowed us to take away all restrictions before anyone else in Europe.
I find it hard to share in the triumphalism. 161,000 Covid deaths (the highest in Europe outside Russia) doesn’t feel like success. The NHS performed well on so many levels, but a combination of austerity and then Covid means the backlog of non-Covid work is huge. And we still have far too many people unwilling to get vaccinated, and too many politicians who seem to think defeating a deadly and unpredictable virus is a matter of political will. As the ‘living with Covid’ plans were laid out, it certainly felt like a shift from days when we were assured science was leading policy.
As a parent and a citizen, I am pleased more normality is returning. But the virus has left me feeling humbled and cautious. I think the Covid generals in government would be wise to be cautious too, because they also know how many surprises this wretched virus has thrown at us along the way. So I will continue to wear a mask on public transport and in shops because I believe the evidence that it reduces (not eliminates) transmission and I don’t want to pass Covid on to a vulnerable person. Even if I wasn’t sure, I wouldn’t take that chance. I will keep testing for the same reason and if I catch Covid (which, unbelievably, I haven’t yet) I will isolate. This is not virtue signalling, I just don’t believe that these are big sacrifices and I don’t feel confident that we’ve ‘beaten’ Covid in the way that word suggests. Without rules freedom discriminates. The vulnerable are not second-class citizens, they deserve freedom as much as the rest of us and if that means that we have to make some minor sacrifices so be it.
Of course we have to learn to live with Covid. But we must never forget how many died from it, nor the families they left behind. We must genuinely learn the lessons, which is why I hope medical voices will be properly heard in the public inquiry. And we should be wary of what Covid might throw at us next. If we equate learning to live with it with thinking it has gone away we create the risk that having won battles, we lose the war.
Jim Down is a consultant in intensive care and anaesthesia in London and author of Life Support, Diary of an ICU doctor on the Frontline of the Covid Crisis.